The "Work Smarter" Myth Cracked (18/18): Stress Response / HPA Axis
Malik was constantly operating in threat mode. Every email notification triggered tension in his shoulders. Every Sponsor request activated anxiety in his chest. Every site delay felt like impending disaster. His Hypothalamic-Pituitary-Adrenal (HPA) axis, the stress response system designed for occasional acute threats, was firing continuously throughout every workday.
The consequences compounded. Malik sleep deteriorated as cortisol remained elevated into evening hours when it should naturally decline. His decision-making quality dropped as chronic HPA activation kept his prefrontal cortex (PFC) partially offline, making strategic thinking nearly impossible. His immune function weakened, leaving his vulnerable to every cold circulating the office. His patience evaporated. Small frustrations that he'd normally handle calmly triggered disproportionate reactions.
Most concerning, Malik couldn't identify when the constant stress had started. There was no single traumatic event, no catastrophic project failure. Just gradual accumulation of typical Clinical Research pressures: Sponsor expectations, site challenges, timeline pressures, budget constraints, regulatory complexity. His brain had learnt to interpret normal work challenges as threats, keeping his HPA axis activated defensively even when no genuine threat existed.
The breaking point came during a routine Sponsor call. The Sponsor asked a straightforward question about recruitment projections. Malik's mind went completely blank. She knew this information intimately, had reviewed it that morning, yet couldn't access it under pressure. His HPA axis was so activated that his PFC had essentially gone offline. The Sponsor waited awkwardly whilst Malik struggled to retrieve information his stressed brain couldn't access.
After the call, Malik sat at his desk fighting tears. He was working harder than ever yet performing worse than ever.
Malik’s manager recognised the pattern immediately: chronic HPA axis activation creating a vicious cycle where stress impaired performance, performance concerns triggered more stress, and the cycle intensified. The solution wasn't working harder or developing thicker skin. It was training Malik’s nervous system to stop overreacting to every challenge.
Understanding the Stress Response
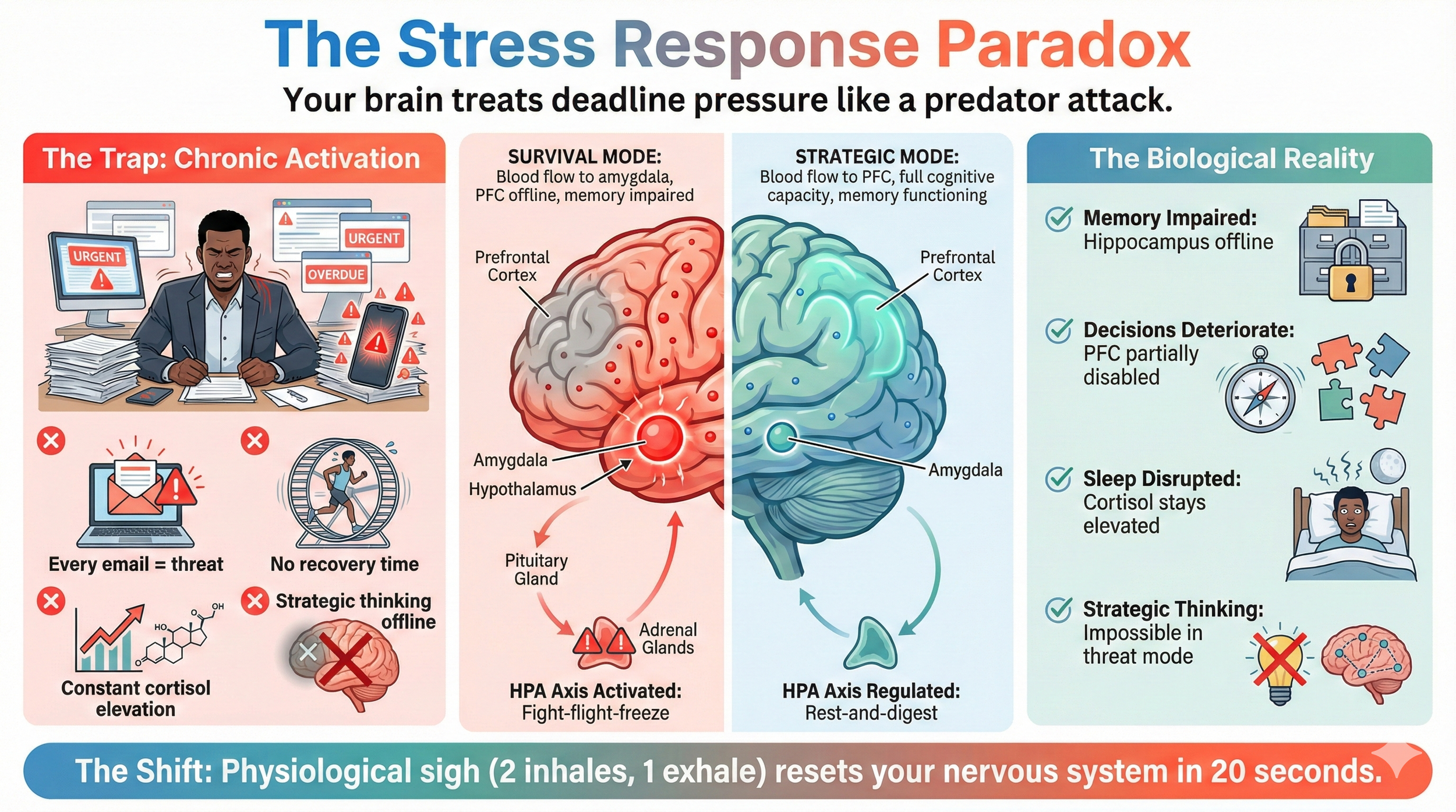
When you perceive threat, your HPA axis activates immediately. Cortisol floods your system. Blood flow shifts away from your PFC (strategic thinking) towards your amygdala (threat response). You enter fight-flight-freeze mode.
This response evolved to help you escape predators, not to help you manage complex Clinical Research projects.
Acute stress that resolves quickly can be helpful, sharpening focus and increasing energy for brief periods. But chronic stress creates ongoing HPA axis activation. Your brain becomes stuck in threat mode. Strategic thinking becomes nearly impossible. Memory, decision-making, immune function, and sleep all become impaired.
Dr Pamela Coburn-Litvak, a PhD neuroscientist with over 25 years researching stress effects on the brain and published in peer-reviewed journals including Neuroscience and Neurobiology of Learning and Behaviour, has demonstrated that chronic stress creates measurable changes in brain structure and function. However, her research also proves that evidence-based neuroscience interventions can break the stress-mental illness connection.
The protocol below applies those same evidence-based principles to Clinical Research project management.
The Protocol
Recognise Threat Response
Learn to identify the physical signs that your HPA axis has activated. You might notice tight shoulders or jaw tension, shallow breathing, racing thoughts, unusual irritability, difficulty concentrating, or a general feeling of being overwhelmed. These are your body's warning signals that you've shifted from strategic mode to survival mode.
The moment you notice these signals, you have a choice. Without intervention, you'll remain in threat mode, making poor decisions and feeling increasingly exhausted. With quick intervention, you can bring your strategic brain back online.
Immediate Reset
Use the physiological sigh technique, which directly downregulates your HPA axis:
Inhale deeply through your nose.
Take a second, smaller inhale to completely fill your lungs.
Then exhale slowly and completely through your mouth.
Repeat this three times.
Research shows this specific breathing pattern calms your nervous system faster than any other technique.
Next, add movement. Stand up, stretch, or take a brief walk. Physical movement helps discharge the stress hormones and signals to your brain that the threat has passed.
Finally, create a perspective shift by asking yourself honestly: "Is this actually threatening my survival?" Usually, the answer is no. The urgent email, the recruitment delay, the budget question—none of these are genuine survival threats. When you consciously recognise this, your brain can stand down from full threat response.
Daily Stress Inoculation
Build resilience through daily practices that keep your baseline stress response calibrated:
In the morning, spend just 5 minutes on controlled breathing or meditation. This isn't about achieving perfect calm; it's about training your nervous system to regulate.
At midday, take a 10-minute walk outside if possible. Exposure to nature has been proven to reduce cortisol levels more effectively than indoor breaks. If you can't get outside, even walking through your building whilst looking away from screens provides benefit.
In the evening, create a 15-minute wind-down routine that signals safety to your brain. This might include gentle stretching, quiet reading, or another calming activity.
The consistency of the routine matters more than the specific activities.
Reframe Stressors
Your brain responds to your interpretation of events, not to objective reality.
Instead of allowing your brain to interpret a deadline as threatening ("This deadline is impossible, I'll never make it, this is a disaster"), consciously reframe it as a manageable challenge ("This deadline is tight, and I can manage it with these specific steps: X, Y, and Z"). The situation hasn't changed. But your brain's response to it shifts dramatically based on the frame you apply.
This isn't positive thinking or denial; it's strategic interpretation that keeps your PFC online so you can solve the problem.
The Transformation
The intervention started with recognition training. Malik needed to identify his body's signals that her HPA axis was activating. For him, the tell was tension in his shoulders and upper back. When that tension appeared, his HPA axis was shifting his from strategic thinking mode to threat response mode. Recognition alone didn't solve the problem, but it gave Malik the awareness needed to intervene before his stress response fully took over.
The physiological sigh became Malik's primary intervention tool. When he noticed shoulder tension, he'd immediately execute 2 inhales through the nose followed by one extended exhale through the mouth. This specific breathing pattern directly signals the parasympathetic nervous system, the branch responsible for calming stress responses. Neuroscience research shows the physiological sigh is the fastest way to down-regulate HPA axis activation. One or 2 cycles, taking perhaps 20 seconds, could shift Malik from threat mode back to strategic thinking mode.
Beyond acute interventions, Malik implemented daily stress inoculation practices designed to keep his baseline HPA activation lower. Morning breathing exercises before opening email signalled safety to his nervous system, priming her for strategic mode rather than reactive mode. Midday walks without his phone provided DMN time and physical movement that reduced accumulated stress. Evening wind-down rituals—reading for twenty minutes before bed, listening to calming music—helped her cortisol levels decline naturally rather than remaining elevated into sleep hours.
Perhaps most importantly, Malik learnt to reframe stressors cognitively. When an email arrived marked "urgent," his automatic interpretation had been "threat requiring immediate defensive response." With training, she began evaluating whether "urgent" meant time-critical or just meant important to the sender. Often, urgent requests could wait until his scheduled communication windows without genuine consequence. Reframing "urgent" as "important and manageable" changed her HPA axis interpretation from threat to challenge.
Three weeks into the intervention, Malik managed the same projects with the same external pressures. But his nervous system response transformed completely.
Email notifications no longer triggered shoulder tension because she'd learnt they didn't represent genuine threats. Sponsor requests became strategic challenges requiring his expertise rather than survival threats requiring defensive responses. Site delays activated problem-solving mode rather than panic mode.
The cognitive impact was dramatic. With his HPA axis no longer constantly activated, Malik's PFC could access its full capacity again. His strategic thinking returned. His memory functioned normally, even under pressure. His decision-making quality improved markedly. His sleep improved, creating positive momentum as better rest supported better stress management.
The Sponsor relationship particularly benefited. When Malik operated in chronic threat mode, she'd approached Sponsor interactions defensively, anticipating criticism and preparing justifications. With his nervous system regulated, she could engage as strategic partner, proactively identifying opportunities and building genuine collaboration. The Sponsor noticed the shift, commenting that Malik had become remarkably confident and solution-oriented.
Malik's reflection captured the essential insight: "You can't eliminate stressors in Clinical Research project management. Sponsor pressure, site challenges, timeline demands—these are inherent to the work. But you can train your HPA axis to not treat every challenge as a survival threat. My work hasn't got easier. My nervous system has got smarter about distinguishing genuine threats from normal professional challenges. The physiological sigh takes twenty seconds. Morning breathing takes five minutes. The midday walk takes thirty minutes. These aren't indulgences—they're essential nervous system training that keeps my brain in strategic thinking mode instead of survival mode. Without them, I'm working harder but thinking worse. With them, I'm working the same hours, but my brain actually functions optimally."
Use the prompts below to help you
How Stress Response Management Connects to Other Brain-Based Strategies
Stress response management enables every other strategy in this toolkit to function effectively:
When your HPA axis is chronically activated and your brain operates in threat mode, your Reticular Activating System filters for dangers rather than opportunities, your Cognitive Load drops significantly as your PFC goes partially offline, and your decision-making quality deteriorates as glucose gets diverted from executive function to survival response.
Flow State becomes nearly impossible when your HPA axis is activated. Flow requires deep calm focus where your entire working memory engages with challenging work. Stress response fragments attention, activates vigilance scanning for threats, and prevents the cognitive immersion flow needs. Professionals struggling to enter flow despite ideal external conditions often discover their HPA axis is subtly activated, creating internal interference that prevents flow regardless of external setup.
Memory Consolidation fails when stress hormones remain elevated. Your hippocampus, essential for transferring information from short-term to long-term storage, is particularly sensitive to cortisol. Chronic HPA activation impairs consolidation even when you're protecting sleep and taking consolidation breaks. This explains why stressed professionals struggle to remember training content despite taking comprehensive notes—the stress response is biochemically interfering with memory formation.
Pattern Recognition requires your PFC integrating information across contexts. When HPA activation keeps your PFC partially offline and shifts processing to your amygdala's threat-focused evaluation, you lose the higher-order synthesis that reveals patterns. Senior professionals under chronic stress often report their expertise seems to disappear—they're not losing knowledge, their HPA activation is preventing access to the prefrontal functions where expertise resides.
Priming Effects become predominantly negative when your HPA axis is chronically activated. You prime for threats, problems, and defensive responses rather than opportunities, possibilities, and strategic partnership. Morning email processing triggers more threat activation when you're already stressed than when you're regulated. The same information primes you completely differently depending on your HPA axis state.
The Default Mode Network cannot function optimally when your HPA axis is activated. DMN synthesis requires relaxed, unfocused attention. Chronic stress keeps you vigilant and scanning for threats, preventing the mental wandering that allows DMN connections to emerge. This explains why stressed professionals rarely experience breakthrough insights—their stress response prevents the cognitive state where insights occur.
Ultradian Rhythms become dysregulated under chronic stress. Your natural ninety-minute cycles of peak performance and recovery get overridden by continuous cortisol elevation. This forces your brain to operate without the rest intervals it needs, creating exhaustion without the recovery that ultradian troughs should provide.
Managing your stress response isn't about eliminating stress or developing emotional detachment. It's about keeping your brain in the operating mode where strategic thinking, memory formation, pattern recognition, decision-making, and relationship building function.
Every strategy in this toolkit works better when your HPA axis is properly regulated because regulated stress response means your PFC stays online doing what it evolved to do: strategic analysis, creative problem-solving, complex decision-making, and relationship management.
Chronic HPA activation hijacks all these functions and redirects your brain towards survival responses that served well for escaping predators but serve poorly for managing Clinical Research projects.
You can train your nervous system, and doing so unlocks every other cognitive capability this toolkit develops.
This is exactly what we work on in my brain-based coaching for Clinical Research project management professionals—training your nervous system to distinguish genuine threats from normal professional challenges, implementing evidence-based interventions that regulate stress response, and creating the neurological conditions where strategic thinking, memory, creativity, and peak performance become your natural operating mode rather than occasional exceptions.